After the diagnosis, we spent the next few days meeting with doctors, and I had to undergo multiple tests to determine the extent of the spread. I don’t believe any of my body parts were left from an investigation at this point.
So my time-management, organizational skills, the work-life balance were all put to the test during this time.

Iron infusion–
Due to the low hemoglobin count, first and foremost, I had to get my iron infusions done. My first iron infusion was a complete disaster. The nurse walked me through the details and the side effects, showed me the snack bar. Then, I was all set to watch a movie and get some iron in. It only took a couple of iron drops — trust me, there is no exaggeration, and I had an adverse reaction to it. If given a checklist of possible side effects, I felt like I could have checked off every single one — my chest tightened, I went pale, my lower back stiffened — multiple things were going wrong for me right there. Next thing, I see about 6–7 nurses and my doctor trying to revive me. After an hour, I drove back home, but what had happened kept flashing in my mind. Robin was not in town, so I called my friend to sleep with me that night. My sisters and Robin’s sister were troubled after hearing what had happened; my friends cried over the zoom call that evening.
Robin got extremely worried, and we cried because he was not there with me — such a terrifying experience. I decided to take an iron supplement instead and eat whatever is required instead of going back for an infusion. Unfortunately, I could not stick to that plan because my oncologist wanted my iron levels to improve significantly before starting chemotherapy. So, I was scheduled for five iron infusions within few days between doctor appointments and tests. They used a different brand for the infusion this time, and it was a huge relief to see my body accept it without any reaction. I was comfortable taking my meetings and carrying out my work during the following iron infusions.
On a funny note — my iron-rich diet with spinach, beetroots, apples, chicken liver, etc., along with the iron infusion, made the stool color a mystery every morning.
Genetic Test-
While everyone speaks about family history, I learned that most people who develop breast cancer have no family history of the disease with my breast cancer diagnosis. I was suggested to do the genetic testing to gain additional information on my mutations and their effect on my children, sisters, and cousins.
BRCA1 and BRCA2 are the two most common genes that can mutate and raise breast and/or ovarian cancer risk. In any of these genes, women who inherit a mutation or abnormal change — from their mothers or their fathers — have much higher-than-average risk of developing breast cancer and/or ovarian cancer.
A genetic test itself involves giving a blood sample. In my case, 47 gene(s) for variants (genetic changes) were evaluated associated with genetic disorders. When combined with family history and other medical results, it helps clarify the individual risk, supports a clinical diagnosis, and assists in developing and managing personalized treatment.
I wish I had recorded the session with my parents discussing the family history — their parents, siblings, and my first cousins. Alternately, I recommend gathering the information from your parents as a fun family exercise, and good luck if your family is as big as my mom’s.
It was much relief to see the test come out NEGATIVE — this means they found no significant genetic changes. It puts my children and family at no risk, puts me at very low risk of developing any other cancer.
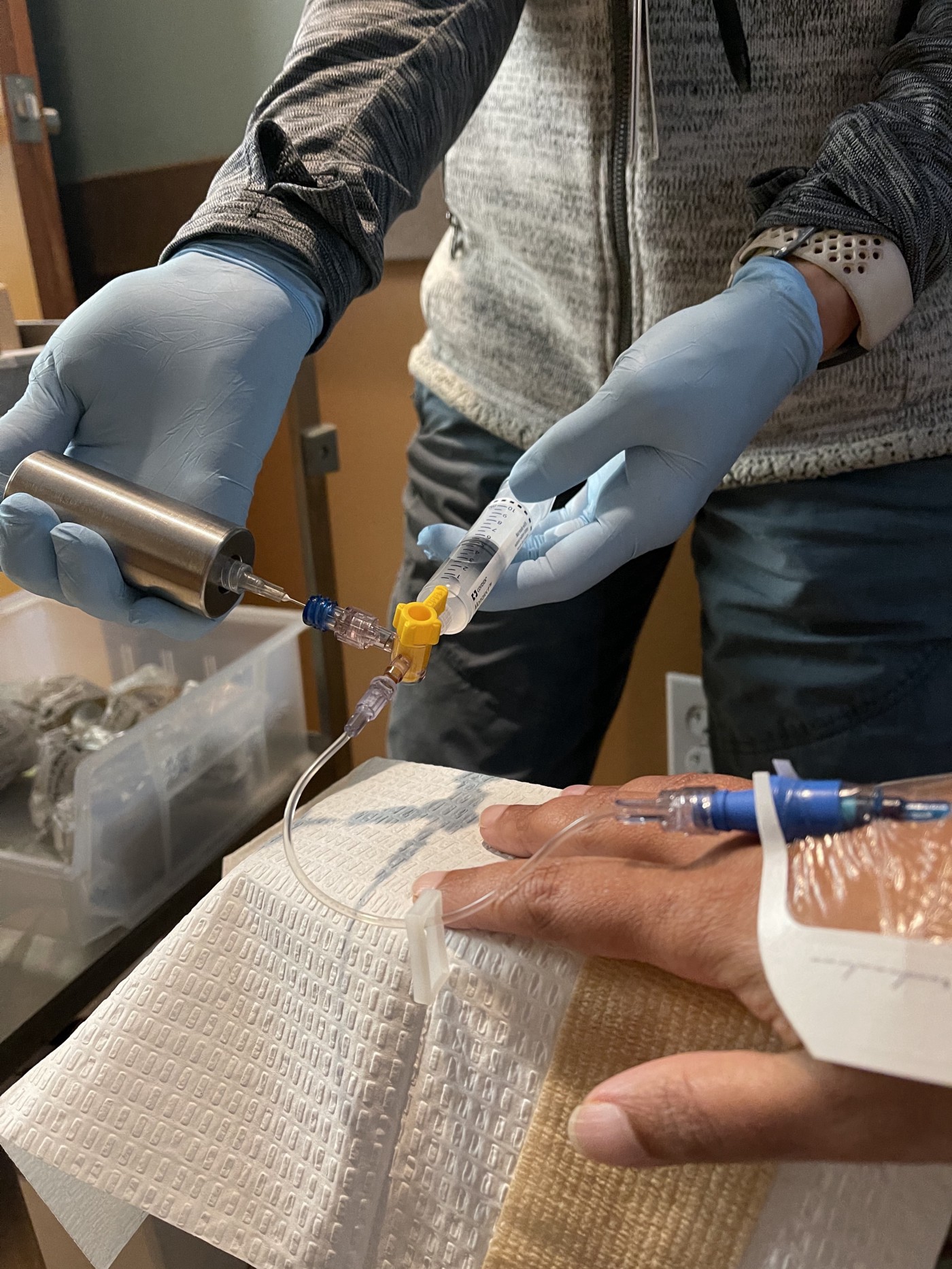
MRI and PETScan-
With multiple iron infusions and blood tests, my veins gave up. They would refuse to take the flush, and most times, the nurses would have a tough time even finding a good nerve. You can see in the pictures — a couple of swollen veins.
The dye injected for the MRI stung me badly, but it was nothing compared to the PETscan I had scheduled for the next day. I have a pretty decent pain-bearing capacity, but in the PETScan, the pain level was excruciating when they injected the dye. By then, the veins were just not ready to take anything more — they were very irritated. I had tears in my eyes as it stung that bad, and the lovely technician came and wiped my tears because I had to remain still to preserve the image. But guess what, there was one teardrop that decided to dangle on my ear lobe, giving me a tickling sensation the entire time. I laugh when I think of it now, but at that time, it split my focus between the possible results of the test and the troublesome teardrop.
Echo Test-
I thought the Echo test was one of the easiest, checking my heart condition before chemo.
Endoscopy and Colonoscopy-
We then met with the gastroenterologist to determine why my iron levels went low. Although the blood work had ruled out internal bleeding, I was still asked to do an endoscopy and a colonoscopy to ensure nothing was missed. During the visit, he also got me to take the breath test. If you have not done one before — trust me, it involved drinking one of the sweetest drinks I have ever had in my life. Growing up in India, our sweets are sweet, but this drink was something else. The evening before the endoscopy and colonoscopy, I had to drink the stomach cleanser, and that kept me busy with the bowel movement the entire night — I would have dropped about 6 pounds that night.
I was back at the hospital at 5:00 am to get a COVID shot and a pregnancy test before the procedure. The nurse had the challenge to find the right vein for anesthesia, and it stung badly again. But only this time, I was not much aware of it. When I woke up after the procedure, knowing I got diagnosed with breast cancer, I kept telling the nurses — I have cancer, and I will fight this out. The nurse and I went back and forth a few times where she kept repeating, — you don’t have cancer but just one tiny polyp, and we took it out. Only when I was fully back to my senses, we both realized we both were telling the right things. I almost felt like a warrior/superwoman ready to enter the battlefield.

Port insertion-
Next, when we met the surgeon, he suggested an outpatient surgery to get the chemo port — the port is my best friend; with all my vein challenges, this is pain-free. A chemo port is a small, implantable reservoir with a thin silicone tube that attaches to a vein. Do a quick search to see how it looks like to visualize it. The main advantage of this vein-access device is to deliver chemotherapy medications directly into the port rather than a vein. I use the numbing cream for blood work and chemo and feel bliss at not having to touch my vein. The port is inserted on my left chest, and the nurse had to find a vein on my right arm for the IV and anesthesia. After several trials and poking, the right arm vein refused to cooperate, so we had to switch arms. It was an inconvenience for my surgeon, but he got the port in beautifully, and my stitches are fully healed.


Amongst all of this, I was due for my second COVID shot.
It was a huge relief to hear from my oncologist that the spread was limited, and cancer is only on my right breast and the lymph nodes under the arm, a locally advanced stage 3-c. Was it truly a relief — nope, but that’s how within nine days, my mindset shifted from knowing I have cancer. One day at a time — had a new meaning in my life. We caught it early, on time, whatever it meant — the annuals helped me with the diagnosis.
We went for a weekend getaway to San Antonio for my daughter’s soccer tournament and enjoyed the much-needed break before starting chemo.

Triple-Negative Breast Cancer Overview and Risks
There are different kinds of breast cancer. My form of cancer, triple-negative breast cancer (TNBC), tests negative for estrogen receptors, progesterone receptors, and excess human epidermal growth factor receptor 2 (HER2) protein. I like how the CDC has explained it — Look at the cancer cells as a house — to get inside to destroy cancer, we must bypass three locks on the front door. If your cancer has any of these three locks, i.e., you test positive for any of them; doctors have a few keys (like hormone therapy or other drugs) they can use to help destroy the cancer cells.
But if you have triple-negative breast cancer, it means those three locks aren’t there. So doctors have fewer keys for treatment. However, chemotherapy is the most effective treatment for triple-negative breast cancer. About 10–20% of breast cancers are triple-negative breast cancers.
Triple-negative breast cancer is considered more aggressive, has a poorer prognosis than other types of breast cancer, and is more likely to spread beyond the breast and more likely to recur (come back) after treatment.
The first five years are crucial after recovery as there is a higher chance of recurrence within the first three years. In addition, it tends to have a higher grade and be more invasive than other types of breast cancer.

Love yourself
After knowing about the diagnosis, many of my friends and family members got their mammograms done — some of them for the first time or after many years. If you have not got your mammogram done, then I urge you to get one immediately. Married/unmarried/with-without kids — doesn’t matter.
Get yours scheduled today.
From diagnosis to the start of my Chemo, everything happened very quickly. Time just flew. However, I often think about if there is anything I would have done differently, knowing what I am getting into with the treatment. I could have; there are always options.
