
Happy Thanksgiving, Everyone!!
I am so grateful to have such fantastic family and friends in my life who I can lean in for anything and everything. It might sound boring as a reader for you to read the Thank You note at the beginning of my blogs but trust me — it gives me immense strength and positive energy from the generous showers of love, prayers, and support!! Could you keep it coming 🙂 Robin, my daughters, and I are sincerely thankful for everything from the bottom of our hearts.
A wreck after meeting the surgeon
I usually read, prepare before a meeting with the surgeon, especially for a surgery of this kind; the typical ME would have read a ton about it. I decided against it this time and went blank and with an open mind to hear out what my surgeon had to say. Robin constantly checked as we were nearing the appointment date. He did that even more on the day of the appointment, including during the drive to the hospital — If I was doing ok, mentally ready to hear about the mastectomy. Genuinely, I thought I was all set because chemo was already taking a toll on me. Still, it almost gave me a drowning feeling when I heard the doctor explain the mastectomy procedure. This had nothing to do with my surgeon — he is one of the best and sweetest doctors that I have come across in my life. He explained the procedure in detail and addressed all my questions exceptionally well. I realized I was not prepared and ready to listen to any of it, or probably it was the fear of having to experience it soon. My oncologist had spoken about mastectomy to me before, so it wasn’t like I was hearing it for the first time. Yet it felt like I was focusing on chemo so much that I almost kept the part of my brain, which had to prepare for surgery, entirely aside. Knowing about mastectomy is one thing, but having to discuss the options with the doctor is different, and it can be overwhelming.

I cried a lot that evening and was an emotional wreck. It was a flash of emotions in front of me, which I find incredibly challenging to articulate and communicate with you all.
Losing both breasts is mentally very hard to come to terms with — it is almost like losing a limb. In such a circumstance, my suggestion is to tell anyone going through it is you are so sorry that that person has to go through this. Would you mind not simplifying and reminding the cancer patient that it’s one step closer to recovery and cancer-free? I am sure every woman is dealing with it differently, and there is no right or wrong way to address it. Whether the woman chooses to be flat or opts for reconstruction, we must prepare without much experience and knowledge of shaping our bodies post-cancer.
I have cried many nights thinking about how it could change me and my life with Robin. I read many articles and blogs about how one could feel — mentally, psychologically, self-image, confidence, depression, negative effects on sex-life — honestly, it could shake your core. The more I thought about it, the more I felt I could probably never come to terms with it. Shower times were getting harder because that is your alone time — the thought of not seeing the breasts eventually was tough to grasp. I did not find much comfort either speaking about it with my mom, sisters, SIL, and friends. Robin and I had heartfelt, candid conversations about this multiple times, and he kept reassuring me that nothing would change between us and breasts don’t define me. However, I was grieving for something that I was born with and used to seeing it for so many years, and now I had to condition my brain to look at me differently — without the breast, nipple, and areola but just a straight-line scar. The anxiety of how it would be waking up after surgery without breasts has kept me awake several nights. As my kids say — scared is an understatement; I was terrified. The mind was going wild with imagination and constantly disputing my preparedness to confront the new-unknown me after the surgery.
My younger daughter was curious about the surgery and learned everything that a 9 yr old could understand. But the conversation with my older daughter (12 yr old) about the surgery went into detail with diagrams and pictures. Her approach, questions, and response were the turning point for me to better prepare for the surgery. She was like a mirror addressing my fear but with the innocence and maturity of a 12-year-old. I started feeling a lot better mentally and did not cry after that night thinking about losing my breasts.
Robin, kids, and I are foodies. We try new things and enjoy all cuisines. During one of these discussions, Robin’s comment was — get your taste back; we want you to start enjoying the food. Knowing him for 25 years, I know he truly meant it! We can live without the breasts but not the taste. I am so happy to have much of my taste back with the chemo cycles ending.

Double Mastectomy and Going Flat — No reconstruction
The recurrence rate of triple-negative breast cancer is very high, so double mastectomy was the best-recommended path to move forward.It was a simple mastectomy on the left breast and a modified radical mastectomy on the right cancer breast.
Simple Mastectomy: In this procedure, the surgeon removes the entire breast, including the nipple, areola, and skin.
Modified radical mastectomy: combines a simple mastectomy with removing the lymph nodes under the arm (called an axillary lymph node dissection). For me, they removed eleven lymph nodes.

I weighed in on the pros and cons of reconstructive surgery and realized that there is no right or wrong decision. It is all about how one sees their comfort and decided not to go ahead with reconstruction and go flat because — I did not want a new variable during the cancer treatment,wanted to heal quickly from surgery and get back to being healthy. I can start using the mastectomy bra, but there are many options to experiment and see what fits them well. I can’t wait to try some of them soon.
I feel so bad for putting my family through so much this year that I want to be back on my feet asap. We have lost a year in my treatment. Even though I brainstormed my thoughts with Robin, it was entirely my decision to go flat. As far as Robin is concerned, he just wants to see me alive and be cancer-free.
Now, after surgery, I am confident with my new body; and recognize as long as there is a will, the body keeps thriving and fighting for you. People around you can give their full support, but you never know whats it’s like until you personally experience it. I did my first Linkedin/ Facebook live session when I resumed my work after three weeks of my surgery. Accepting the new me was necessary; the marks of fighting breast cancer shall remain — the scars don’t matter; I am still beautiful immaterial of the breasts not being there on my chest anymore. The heart is still the same, and I am proud to bravely embrace my decision to go flat.

Surgery and Recovery
As the surgery days were nearing, I started wrapping things at work because I planned a 3-week medical break for recovery. My vitals looked good after chemo, and physically and mentally, I was ready for the surgery. It was a 3-hour surgery, my first big surgery, so there was a bit of anxiety about it. My sister had come down a couple of days before to help us out.
The night before the surgery, I worked out and could keep my calm. Robin, my sister, and I decided to burn my old bra in the backyard — it had no significance yet meant a lot. As instructed by the surgery team, I took a shower at night and the morning of surgery with the antibacterial surgical soap. I even managed a good 4 hour sound sleep the night before the surgery. We reached the hospital by 5.30 am, and the prep started almost immediately. I felt good positive vibes from the nurses, anesthetists, and the surgeon that morning. At home, the kids were with my sister but woke up before I left for the hospital, and the older one was texting Robin to know how I was doing before and after surgery.


The surgery went well, and in the recovery room, I could feel nothing when I woke up — none of the nightmares about waking up without breasts after surgery was real. There was discomfort in the chest area, and the pain meds and anesthesia kept me loopy and sleepy almost till late evening. The breast is separated from subcutaneous tissue and muscle during a mastectomy, resulting in a raw surface that leaks fluid called serous fluid. Although serous fluid production is normal, the doctors don’t want the fluid to stay inside and want it to come out, so a drain is placed. There are different types of drains. For me, the Jackson-Pratt or JP drain was used. I had two drainpipes on each side tucked away nicely in the top that my lovely neighbor had gifted me. As the tissues grow together, the fluid production slows down and eventually stops. This process takes about 14 days. Once drain production is less than 1 ounce (30 ml or 30 cc) in 24 hours, the drain can be removed. (https://www.breastinstitutehouston.com/post-mastectomy-wound-care/)
https://www.healincomfort.com sells the special drainpipe shirt and is a great gift for anyone going through mastectomy.


The patho results from the surgery looked promising — out of the eleven lymph nodes, only one came out positive, and there was a couple of remanence of 3 mm cancer cells from the right breast that we took out.

It was tough to get up that morning because of having to lift the upper body without much balance, which previously the breasts were giving — it came down to the core strength. The occupational therapist came in and helped me get up, walk around a bit, and taught me the hand exercises to be done the next few days to increase the range of motion on both my arms. She was extremely friendly and knew her job well. Although I had to take an additional painkiller on the surgery night, overall, my pain was under much control.

The first few days, the numbing effect in the surgical area kept me relaxed, and I could sleep well. However, after five days, one of the drainpipes on the right started hurting. I walked around and continued doing the motion exercises. The pain began to worsen, but luckily the fluid output had reduced, and the doctor could get it out on the 7th day. So one drain pipe on each side came out on the 7th day, but the previous night, I could not sleep because of the pain. Every time you move, breathe, it would hurt. I was relieved to see the pipes come out.
For the next few days, I continued doing my minimum activities without any painkillers. At the hospital, my sister helped me shower, then at home Robin would help me with showering and dressing up. Lifting the right arm would give a terrible pain because of the removal of the lymph nodes. So I had to get help to put soap, hold the drainpipe while showering, etc. The fluid also had to be measured and recorded twice every day, and Robin, my sister, and the kids would take turns to empty the drain.
After ten days, the second drainpipe on the right chest started to give me trouble. Friday and Saturday nights were again excruciating, and I could not sleep a wink. I couldn’t hold my tears on Saturday night, and Robin tried to help me a lot, but nothing worked. The entire night, I had contraction-like pain in the surgical area occurring every few seconds, and the drainpipe gave me poking pain. It was almost like someone constantly rubbing an open wound. I have an excellent pain-bearing capacity, but this was almost beyond ten on a pain scale. Tylenol was of no help. So the following day, on Sunday, we decided to go to the emergency as I also felt a fluid discharge from the skin near the drain pipe.

They checked the discharge in the emergency, thought it could be an infection, and advised me to stay back that night in the hospital. To treat the infection, they had to give me IV antibiotics and, of course, do my blood work. A new challenge started now to find my vein. After several attempts, the nurse decided to bring in the vein finder, and even with that, we were not successful in finding the vein. They poked my port twice, and the port was also not supportive that day; we could not draw any blood from it. Finally, they decided to give me an ultrasound IV but right before they could get the machine the nurse could get a vein — YAY, that was such a big win for the team and me to get a vein finally.
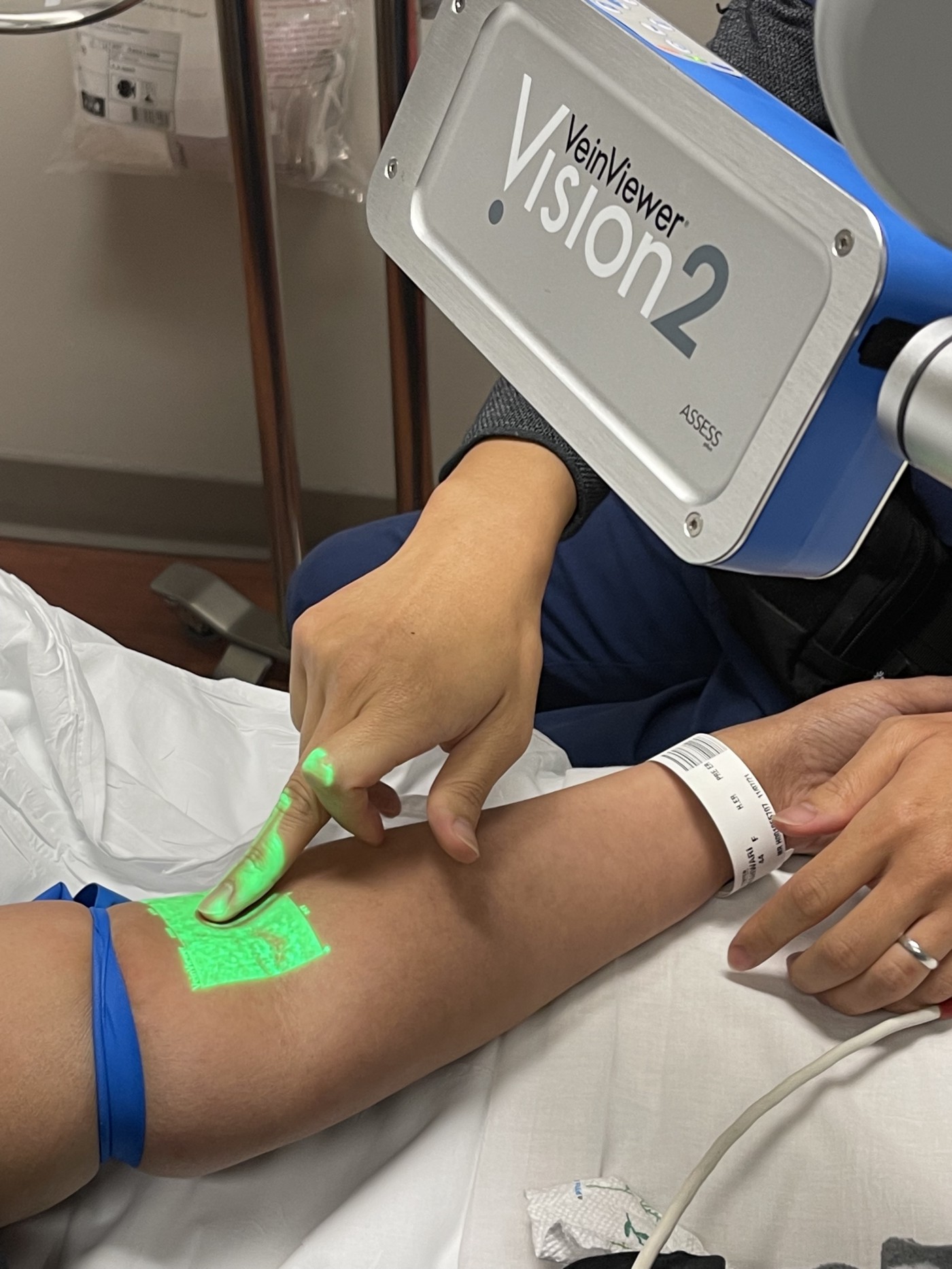
They drew the blood first and then started the painkillers and antibiotics. The strong painkillers put me in the loop, and Robin told me I blabbered a lot. I spoke about everyone (check with him if I mentioned anything about you), including my deceased mother-in-law, giving me her blessing and asking me to rest. That night, the nurses gave me Norco and Morphine combined every 4 hours, but my pain continued. Because there was still fluid collecting in the drain pipe, they could not get the drain pipe out. Finally, Monday afternoon, the pipes came out after 14 days, and I was in immense relief. The antibiotics continued, and I slept well for the next several hours before getting discharged the following day. I was trying to beat the pain with Tylenol, that Norco and Morphine combined could not do it.
Halloween, Diwali, and Thanksgiving — all came during this one month of my recovery from surgery. My friends sent food for a week and wouldn’t take a NO for an answer to help my mom. I resumed work after three weeks and am healing well now. I managed to step out for some shopping with family this long weekend. There is swelling and discomfort, but I know how to deal with it now. I randomly get the nerve-tingling pain on the right hand, but I still do not feel the sensation under my armpits on the right side. I feel itchy when I sweat, a side-effect of chemo that is continuing, but happy to be able to do my Peloton every day.


Being Thanksgiving week, there are just numerous things that I am thankful for, but most importantly, it is all you, my fantastic family and friends, your generous love that is giving me the strength to fight this battle.
What’s Next?
See you all in the New Year!! I start the radiation treatment from the last week of November, and it will go till January 2022. I wish everyone of you a fabulous, joyful, and healthy holiday season.
