
This blog was way overdue. I wanted to write after wrapping up my treatment, but one thing led to another, taking my focus away from writing. I was considered cancer-free after the surgery when the breast and lymph nodes were removed. The radiation therapy was preventive. We were waiting for the lab results from the mastectomy to know how much radiation would be required — it is similar to a medical prescription. So with some residual cancer cells in the breast and one of the lymph nodes, 33 sessions were decided — 28 on the right breast area and five on the surgery scar line.


The radiology team was truly outstanding. The radiation took place every day — Monday to Friday for ten minutes. During the first appointment, the radiation team creates a mold on the bed to ensure the measurements perfectly align with your body and the machine. The process is a bit bizarre — with a routine to follow daily. You check in, change your outfit, get into the radiation room, lie down for 10 minutes under the machine, and then done. Music is playing in the radiation room, an artificial skyline above your head, making everything as comfortable as possible. You meet the same patients for a certain period depending on the length of their treatment. For the entire two months of the therapy, 2.30 in the afternoon, which was my appointment time, would make me uneasy. During the week of Christmas, the team worked extra hours to accommodate us for the holiday. So I got an appointment at 6 am — showing their passion and interest to keep us cancer free. I was just blown away by this level of commitment. At the end of the treatment, although I was happy not to get into the room again, I missed meeting the team of nurses and radiation technicians and sharing my weekend plans.
After 16 chemo cycles and a double mastectomy, the radiation team told me the treatment would be much easier to manage. True, I did not feel much more than occasional fatigue for the first couple of weeks. I would actually plan during my drive to the clinic about what I wanted to focus on when I had to lie down under the machine — sometimes it would be my work-related, some about certain chores at home — almost every day, I had a new topic to think and act on during the session. The goal was to avoid thinking about cancer or the damage the machine was doing to my skin.


I had my sisters, nieces, nephews, and parents at home for Christmas and New Year. My niece and nephew decided to spend the holiday season with us from India. Although I couldn’t join them everywhere, I managed to spend as much time as possible. It was an excellent distraction for Robin, me, and the kids. I still remember what my doctor told me, knowing there would be 16 of them at home for a week. Chemo is harsh, surgery is difficult, radiation is hard, but having 16 family members at home is worse — play your cancer card and ask them to do everything around 🙂 . Now, I hope to get the crazy times again with all of them real soon.

Even though it was wintertime, I drank a lot of water to avoid dehydration, maintain a healthy diet, and continue my peloton biking to re-energize. By week four, I would feel nauseous some days, and ten-minute power nap sessions in the evening helped me a lot. From day one of the treatment, I diligently applied the radiation cream as suggested. After a couple of weeks, when the skin started showing a little bit of irritation, I also incorporated cold-pressed coconut oil at night to keep the skin moist for a long time. By 3rd week, I was so used to applying the cream every few hours that one day in the morning, by habit, instead of the toothpaste, I ended up with the cream on the brush.


After week three, the skin irritation started to show up, and my right breast area began to resemble a tandoori chicken — RED :).From the end of December till almost the end of February, I could not do the peloton to avoid itching and sweat in my radiation area. From January, the skin started getting worse, peeling, and painful. I resorted to cotton tops during the entire radiation process until the new skin came in. It takes a toll on your clothing because of the cream and dry skin sticking to it. Even now, after seven months of the treatment, the skin is dark in that area. There is still no hair in the armpit area, and the entire area gets tightened periodically. Vitamin E oil messages around that area helped in rejuvenating the tissues under the skin. Robin has helped me several nights with the massages to ease the skin.
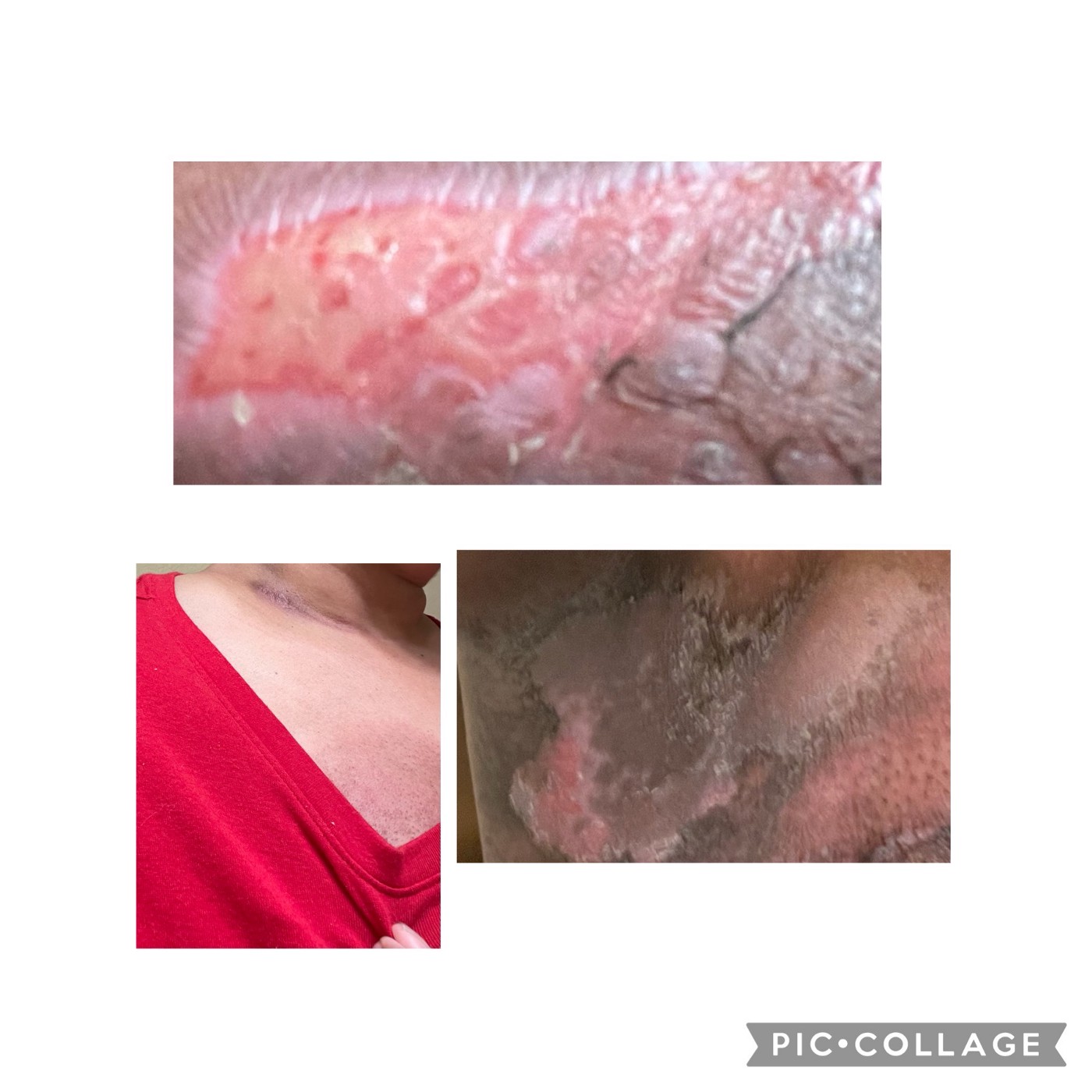

My immunotherapy treatment continued during the radiation therapy, so I also had that going every three weeks.

With radiation and mastectomy surgery, your posture gets altered because you no longer have the breast to give the support, something that we all are born with, and over the years, those tissues help balance our shoulders and the back. Also, with the lymph node removal — one is highly prone to Lymphedema. Both, in combination, would give me shooting pain in the right arm joint, which was taking a lot of strain. Now, I had to re-learn how to use the other muscles in the body to give the proper support without causing much damage to the shoulder bones.
Although I was warned that it would take a couple of months to heal from the radiation, just when I thought I was nearing the finish line, I learned that I would have to undergo a few sessions of physical therapy to deal with Lymphedema. It is easy to feel disappointed and discouraged and give up on the treatment. Patience, determination, and perseverance have a whole new meaning with cancer, and every phase of the treatment cycle never shied away from reminding me about it. I felt accepting and acknowledging the new normal was essential to be sane and to sail through the process.
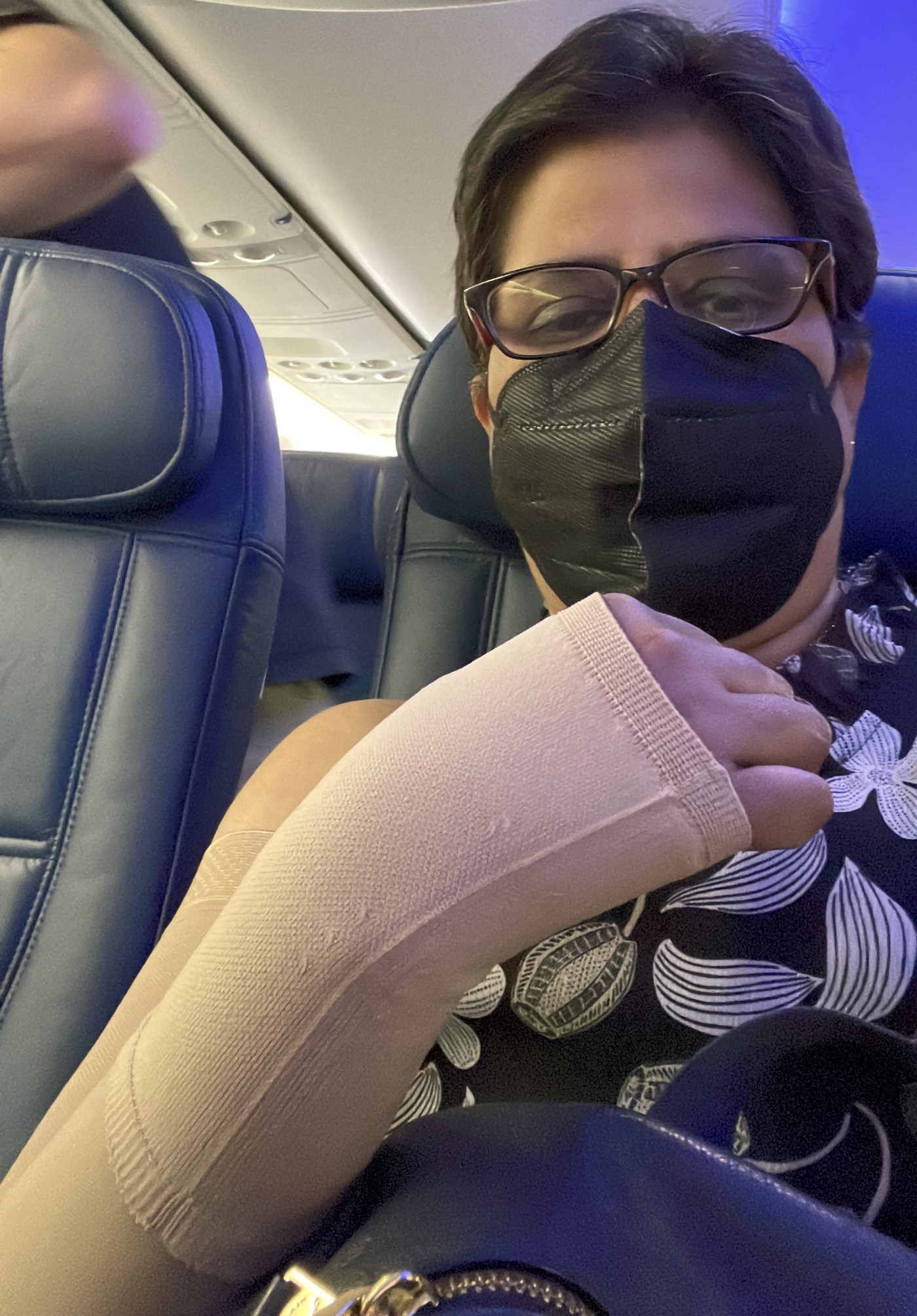
What is Lymphedema? It is a build-up of lymph fluid under your skin, causing swelling and discomfort, and in the absence of lymph nodes, the fluid cannot drain on its own. So during the physical therapy sessions, my therapist would drain the fluids manually and teach me exercises to use my back and shoulder muscles effectively to avoid any ergo pain. She taught me to recognize fluid accumulation, swelling, stiffness, etc., managing the self-drainage of the fluid to feel comfortable.
For the curious readers — here is the link to view the self-drainage video
https://www.compressionguru.com/klose-training-self-manual-lymph-drainage-dvd
I have also taught Robin how he can help me with Lymphedema drainage, so periodically, when I get swelling, he also helps me with the drainage even now.

I wrapped up my radiations in mid-January, immunotherapy in May, and physical therapy in mid-June. When I think about it, there was a genuine calmness and peace within me, knowing my treatment ended, my numbers were looking good, and overall I was feeling good about my health. We made a road trip during the kids’ spring break in March to San Diego and LA and enjoyed our stay at one of our friend’s houses in San Diego.
I was coping with the fatigue part but with being back on my peloton, having an appetite started to give me a sense of normalcy. Until one of our friends invited us for dinner at her place in Austin- with about 8–9 families, and for the first time in two years with COVID and my cancer condition- I met them all together. I was extremely overwhelmed, and a few conversations with friends brought tears to my eyes streaming down — making me an emotional wreck. Robin suggested we head home, seeing me uncomfortable, but I did not want to give up and decided to stay closer to him the entire evening. I was still disturbed by my experience because that is so not me — I could not fathom the thought of not being able to connect and talk with my friends. I brought it up with my oncologist during my follow-up appointment. During the conversation, I realized that I was in the post-menopausal phase with my treatment plan to date. I experienced hot flashes and severe itching with sweat, but I did not care to think much about it with the chemo, radiation, and surgery. When the treatment ended, some of these side effects were more prominent, so the anxiety levels were high.

On the day of my last treatment, Robin was with me at the doctor’s office, and I just cried knowing I didn’t have to come for the infusions — I felt on top of the world with the new life and looked forward to continuing making some fantastic memories. With the COVID cases still on high earlier in the year, Robin was not allowed in the infusion area, so I read the proclamation on the wall and rang the bell to celebrate the end of treatment. Kids also joined us and were waiting in the parking lot for me. We went for Sushi — one of our family’s favorite food and friends stopped by in the evening for a small celebration.

Over the next few weeks, it was an emotional roller coaster. I cried some days for no reason; there was a struggle to be back to everyday life — the original normal. The cancer journey and the side effects from the treatment messed me up, and getting torn between the old, and the new normal made me feel frustrated, have mood swings, and look deep within my core at who I truly am. My priorities and perspective on life, however, are changed forever.
Robin kept reminding me that it would take time for me to recover, and after reading articles and speaking with cancer survivors, I realized that I was not alone in feeling this way. As I write this, I struggle to express myself. I can only say to be empathetic around the cancer patient; there is nothing that the person going through it can do to help you with your emotions and feelings. The caregivers and support system have to figure out a way to deal with their individual situations. As harsh as it may sound when you read this, it is a painful truth.
The cancer journey is traumatic. I am tricked again by my thoughts of everything good finally alleviating, only to be disillusioned. The happiness was short-lived.

